Asthma Inhalers
Background on Asthma Treatments
The treatment of asthma has changed significantly over the past century. It was treated primarily with oral medications through the first half of the 20th century. The medications are then absorbed from the stomach and bowels and are sent to the lung and every organ of the body. This can produce a large number of side effects. Since most asthma medications are related to adrenaline, there is a common side effect of all “uppers” to increase blood pressure, heart rate, as well as the side-effects on the brain, muscles of the GI tract including its sphincters. As these adrenergic drugs, or beta-agonists, are refined, each generation of new drugs has less of these side effects and more bronchodilator effects on the bronchioles of the lungs.
The oral asthma drugs were of two categories. In addition to the adrenergic drugs above, which include Isuprel and Epinephrine, there are the Methylxanthines or theophylline.
Methylxanthines (such as theophylline) were once widely used, but do not add significantly to the effects of inhaled beta-agonists. They are still used in special circumstances. Theophylline is sold under the brand names Uniphyl, Theo-Dur, Slo-Bid, and Theo-24 and is available as an oral (pill and liquid) or intravenous (through the vein), or as a rectal suppository. Theophylline is long-acting and prevents asthma attacks. Theophylline is used to treat difficult-to-control or severe asthma and must be taken daily. The intravenous preparation is sometimes used to break a severe status asthmaticus, a life threatening asthma crises.
Some asthmatics because of disabilities, mental incapacities, or other infirmaties are unable to use nebulizers or the modern MDIs and thus are given pills, either beta-agonist or methylxanthines, as the best treatment options.
Nebulized asthma drugs
In the mid twentieth century, nebulizers came into vogue. Before the invention of the Metered Dose Inhalers (MDI) asthma medication was delivered using a squeeze bulb nebulizer which was fragile and unreliable. These were basically a glass bulb apparatus into which liquid medications was placed and then atomized or nebulize with a rubber hand squeezed bulb.
The relatively crude nature of these devices also meant that the particles that they generated were relatively large, too large for effective drug delivery to the small airways of the lungs. Nonetheless these nebulisers paved the way for inhalation drug delivery providing the inspiration for the MDI.
The metered dose inhaler
MDI’s were first developed in 1955 by Riker Laboratories, now a subsidiary of 3M Healthcare. At that time MDI’s represented a convergence of two relatively new technologies, the CFC propellant and the Meshburg metering valve which was originally designed for dispensing perfume.http://en.wikipedia.org/wiki/Metered-dose_inhaler – cite_note-Clark_1995-5#cite_note-Clark_1995-5 The initial design by Riker used a glass canister coated with a vinyl plastic to improve its resilience.http://en.wikipedia.org/wiki/Metered-dose_inhaler – cite_note-Purewal_1997-4#cite_note-Purewal_1997-4 By 1956 Riker had developed two MDI based products, the Medihaler-Epi containing epinephrine and the Medihaler-Iso containing Isoproterenal or Isuprel.http://en.wikipedia.org/wiki/Metered-dose_inhaler – cite_note-EoPT-1#cite_note-EoPT-1 Both products are Beta agonists which provide short term relief from asthma symptoms. For the long time asthma sufferers, these devices are well known as the Isuprel Mistometer of the 1950s to the Bronchometers of the 1960s. The Isuprel Mistometer is now an OTC product available to anyone without a prescription. It is a very short acting bronchodilator on the order of 30 minutes to one hour. It must be used with caution since it still has all the major cardiac side effects.
Isuprel gave way to Bronchosol, Alupent and Albuterol, each with about an hour’s longer duration of action than the previous. Albuterol has now largely replaced all predecessors in the short term treatment of asthma. Its effect lasts 4 to 6 hours. This in turn has largely been replaced by salbutamol, or salmeterol or Serevent which is more beta selective and has a longer duration of action. Its effects last from 9 to 15 hours. This drug allow severe asthmatics to sleep through the entire night with awakening for more inhalations before daybreak.
Albuterol has remained as the preferred rescue medications for exacerbations of asthma. Although considered short term or rescue therapy, a treatment should last between four and six hours. During an active asthma attack, this may need to be given every two hours or even every hour until the attack resolves. If it doesn’t resolve after two or three treatments, a dose of steroids may be required. Every asthmatic has a bottle of prednisone at home for just such emergencies which may then negate a rush to the hospital. At the hospital they will be giving the equivalent of 40 to 80 or even 125 mg of prednisone (Solumedrol) intravenously. Hence, asthmatics know that 40 mg is frequently the initial dose they give themselves which may need to be repeated in 4 to 6 hours. They should obtain their doctors guidance and approval of this. This one of the instances when Theophylline is still given also. You may want to give your physician a copy of this report and obtain his variations of this treatment.
Corticoid Steroid Medications
Cortisone congeners including prednisone have been used for a long time in all atopic or immune diseases of which asthma is one. If the standard bronchodilators as outlined above are not controlling the asthma, suppression of the immune system may be required. This also suppresses the adrenal glands. Hence, long term use may cause adrenal atrophy and lead to dependence on steroids as life saving. In addition to adrenal atrophy, it may cause osteoporosis, cataracts, and paper thin fragile skin. Much of this can be avoided in those patients requiring long term steroid therapy by giving prednisone on an every other day schedule. This gives a jolt to the immune system every other morning and then allows the adrenals to recover over the next 36 hours so they don’t atrophy.
Steroid inhalers
Concurrent with the short and long acting beta-agonist, the steroid inhalers have developed in a similar pattern. They have included AeroBID, Azmacort, Fluticasone, Mometasone, Budesonide and others. These are now being incorporated into a single MDI with the long acting beta-agonist for their anti-inflammatory effect (Advair: Fluticasone and Serevent; Symbicort: Budesonide and Formoterol; Dulera: Mometasone and Formoterol). This has further revolutionize asthma treatment to allow reformulation of damaged airways and reverse the downward course of many asthmatics.
Respiratory Therapy
Motor driven nebulizers were then developed which required respiratory therapists in the hospital to give regular or even continuous treatments to patients. They were the experts in mixing medications for the nebulizer bulb and administering it to patient on an every two, three, four or six hour basis each day. They could observe the responses and provide the physician feedback on how the treatment could be more effective.
The mixing has now been simplified by ampules of albuterol or combination products, which patients at home can put in the nebulizer. This has revolutionize home therapy.
How to effectively take an MDI treatment at home
When seeing a patient with a poor response to the inhaled medications, the doctor always asks the patient to demonstrate how he or she takes the medication. It has been shown that about three-fourths of patients never deliver the medication effectively to the entire lungs. By observing the patient, one can tell if the delivery was just to the tongue or throat and or did any of it reached the top portions of their lung or the lower portions of their lungs near their waist line. “Topping off” does not treat the asthma.
Empty your Lungs or Expell the air in your lungs first before you squeeze the MDI!
One can never fill the lung with aerosols unless one empties the lungs first. Hence, one must fully exhale, (blow out) and then open his or her mouth in front of a mirror and press the nebulizer concurrently with starting inhalation. One can watch the flow of aerosolized medication go directly to the back of the throat and disappear into the trachea and the lungs. One must then hold his or her breath for 30 seconds or more to give the medication time to be absorbed by the bronchials. The medication is rather expensive and hence one should not waste it by expelling it into the atmosphere before it enters the alveoli and the capillaries in the lungs. This takes 20 to 30 seconds or more. Swimmers are normally able to hold their breaths for a minute or two.
Illustrations
With the lips tight around the mouth piece as shown in this example the medication is delivered primarily to the tongue, gums, teeth, buccal the throat membranes unless there is a high flow of air around the canister to propel it past these structures. Hence, it is better to have your mouth open and watch the medication being delivered properly in front of a mirror.

In this example, there may be a vigorous inhalation of air around the Nebulizer through the partially opened mouth and the medications may reach the lung. This can be determined reasonably accurately by watching this lady give herself a treatment. If she then holds her breath for 30 or more seconds, this may deliver the aerosol to her lungs.
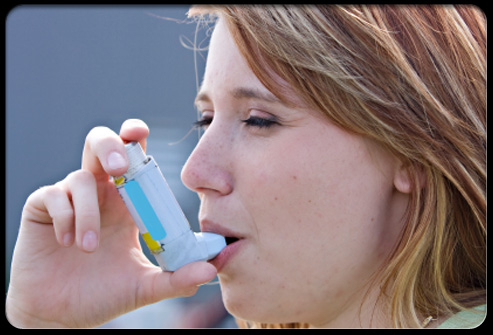
This young girl is taking the aerosol with her mouth open and eyes closed. The mouth piece is resting on her lower teeth and it would appear the aerosol is directed directly to her tongue. It would be better if she held the mouth piece against her upper teeth for a more direct aim to her glottis and windpipe. She appears to be following the directions given her as a good student, and should be taught to observe herself in a mirror until she has the technique mastered.

Albuterol inhaler
As governed by the 1987 Montreal Protocol on Substances that Deplete the Ozone Layer, all inhalers that contain CFCs have been discontinued since 2010 under the auspices of the UN Environment Programme. As a consequence of the Montreal protocol, the first companies to patent an inhaler formulation containing HFAs are Riker for the HFA134a in 1989 and Hoescht for the HFA227 in 1990. These patents are now expired.

ProAirHFA
One of the new hydrofluoralkanes (HFA) inhalers
which is free of chlorofluorocarbon (CFC).
The Advair Diskus inhaler comes in three dosages. The 100 mg of Fluticasone, the 250 mg of Fluticasone, (the most common dose used) and the 500 mg of Fluticasone each with 50 mg of Salmeterol or long acting bronchodilators.
Instructions for Advair Diskus
- Check the remaining number of doses on the Advair Diskus, located just below the thumb rest. Be sure that there are still doses in the diskus.
- If there are remaining doses, push the lighter half of the diskus backward, using the
thumb rest. This should reveal the mouthpiece and dispenser lever. - Make sure the mouthpiece is facing upward. Pull the lever backward. This should open a small door beyond the mouthpiece, allowing access to the dose of medicine.
- After emptying your lungs by expelling all air, place your mouth tightly over mouthpiece and inhale deeply.
- Remove mouthpiece and hold your breath for a minimum of 30 seconds or as long as you can with your lungs filled with the medication.
- Exhale the spent aerosol.
- Flip the diskus back into the closed position. Check to make sure the dosage has gone down one number.
Read more: How to Use an Advair Diskus | eHow.com http://www.ehow.com/how_4516865_use-advair-diskus.html#ixzz1MSTV6VuG
Delbert H Meyer, MD
Pulmonary Medicine
6945 Fair Oaks Blvd, Ste A-2
Carmichael, CA 95608
916-488-5864
See Blog at www.DelMeyer.net
Archives at www.delmeyer.net/MedInfoHealthLine